1. His Choice Vasectomy: No needle, no scalpel and one visit!
I was the first doctor in the Carolinas to offer men His Choice Vasectomy: no-needle, no-scalpel, minimally invasive vasectomy with the option of having their vasectomy performed during a single office visit.
My goal is to provide the most minimally invasive vasectomy procedure. I provide vasectomy without a needle to administer anesthesia and without a knife to make a skin opening. All of this can be done with a single office visit. A consultation is not always required.
We do our best to make your visit as efficient and as painless as possible.
2. Open ended vasectomy technique
I use an open ended vasectomy technique. Older, conventional vasectomy techniques have been associated with more vasectomy complications. An open ended vasectomy technique may cause less discomfort after vasectomy.
More Information: Open ended vasectomy technique
3. Sedation vasectomy if requested
Most men can have vasectomy without the need for anti-anxiety medication or narcotic pain medication before, during, or after a vasectomy procedure. The vast majority of men can have vasectomy safely and comfortably with local anesthesia alone.
I now offer vasectomy with deep sedation if requested.
More information: Vasectomy with deep sedation
Sedation vasectomy is not necessary but neither is flying first class nor sitting in a luxury box at a sporting event!
Some men will chose to have sedation vasectomy for the extra guarantee of comfort sedation can provide.
4. Experienced vasectomy doctor with great after vasectomy statistics
As of January 1st, 2025, I have performed over 8,141 vasectomy procedures.
I have also performed vasectomy internationally in the Philippines, Kenya, and Haiti. The following links will provide more information about those mission trips.
We keep great vasectomy statistics demonstrating the safety and acceptability of His Choice Vasectomy:
5. Offering vasectomy without judgement!
I only have two requirements for patients when having a vasectomy at my practice:
- They must be over the age of 21
- They must be able to provide informed consent
I do not require you be married, obtain spousal consent, bring your partner or a driver, have a minimum number of children, have a psychological evaluation, or wait a minimum number of days after you make your decision.
My patients are adults and have the ability to make their own decisions about what is right for them.
6. Office visits? Your choice: One or two? Little wait time for appointments
I offer patients a choice of two appointment types when having a vasectomy.
- Having their vasectomy performed all at one visit*
- Having a vasectomy consultation first and then returning to have the vasectomy performed at a later visit.
I am the only provider who offers men the choice of having the vasectomy done during a single office visit.
More Insight on how many visits are required for vasectomy
* Even when having a single visit vasectomy procedure, I will meet with patients in the consultation room to answer important questions before the vasectomy procedure.
Dedicated Vasectomy Time: My time is important...your time is important
When you call my office you can usually have a vasectomy within 2 weeks of calling to schedule an appointment.
My goal is to not make patients wait more than two weeks. Many offices won't provide you with timely appointments and will require you wait for several weeks before you can have either your consultation appointment or vasectomy procedure.
I dedicate my office time on Thursdays and Fridays and exclusively provide vasectomy. This means when you come for vasectomy you will have a quick and efficient visit. You won't be delayed because I am stuck in the operating room, rounding in the hospital, or taking care of some unexpected emergency.
7. Affordable vasectomy
I offer one of the most affordable vasectomy procedures around.
The cost for a vasectomy procedure is $1,250.
You will need to pay in full on the day of service for your procedure. We do not accept health insurance as payment for vasectomy but you can submit for reimbursement from your health insurance company after the procedure has been completed.
Most men, even those with health insurance, will pay less when having a vasectomy at our office than with many other providers. Most doctors require two appointments and the average cost for vasectomy is $1,500 in North Carolina and $2,500 in Virginia.
For more information: Cost of vasectomy and health insurance coverage and reimbursement
We will provide you with the information required so you may obtain reimbursement directly from your health insurance company after your vasectomy has been completed. It is not that difficult to obtain reimbursement directly from your health insurance company and they will be more responsive to you since you are their paying client.
8. No follow-up visit required
I do not require a mandatory follow-up visit after vasectomy because the overwhelming majority of vasectomy follow-up visits are unnecessary.
Every patient will be provided my personal cell phone number should they feel they are having a problem that requires urgent attention. Patients are also encouraged to call my office and speak with our nursing staff if they have a concern.
We readily answer the phone at our office...no menus to navigate and you can easily and quickly speak to a real person!
Patients who have concerns after vasectomy can easily obtain a follow-up visit should they feel it is important.
9. Flexible semen sample testing
I offer four choices for completing the 3 month post-vasectomy semen sample test:
- Returning to the office for semen sample testing
- Having it done at a laboratory close to your home
- Mailing your sample to my office for evaluation
- FDA approved home after vasectomy home testing kit (SpermCheck)
10. Great vasectomy videos! Great patient reviews!
Our goal is to make your vasectomy as easy as possible. We want your visit to be informative, efficient, and with minimal wait time.
To provide better information for patients, we have developed a 9 part vasectomy educational video series:
Our patients recognize the great service we have provide and our Google Reviews prove it:
—–
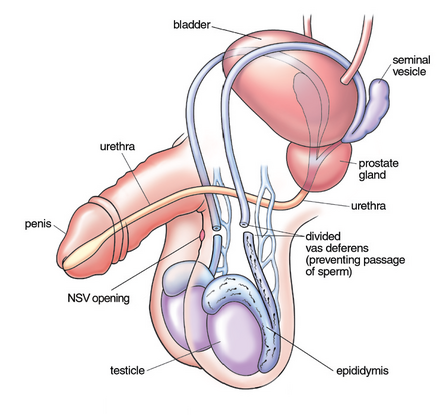
How Does Vasectomy Work? Facts vs. Myths
Vasectomy does one thing... and one thing only. Vasectomy prevents you from having an unplanned pregnancy.
Many of us have a very limited understanding of our anatomy and human reproduction. It is amazing how many myths exist about vasectomy.
For a more extensive understanding visit: How Does Vasectomy Work? Facts vs. Myths
Vasectomy does not make you less of a man, does not decrease testosterone levels, does not cause prostate cancer, will make you sing soprano, and will not cause your testicles to fall off.
What Is His Choice Vasectomy?
His Choice Vasectomy: No Needle No Scalpel
His Choice Vasectomy is one of the most minimally invasive vasectomy technique. His Choice vasectomy means the following:
- No needle used for anesthesia
- No scalpel used for skin opening
- Single opening in the middle
- Open ended technique
- 72 hour long acting local anesthetic administered
For more detailed information: His Choice Vasectomy Explained In Detail
His Choice Vasectomy is the best and most minimally invasive vasectomy procedure available. In order to understand why His Choice Vasectomy is the best vasectomy procedure, then you should understand the alternative vasectomy procedures.
For more detailed information: Different types of vasectomy procedures
Risks of Vasectomy
Vasectomy is a safe procedure with a very low risk of serious complications and a very low risk of causing long term problems.
For more detailed information: Risks of vasectomy
His Choice Vasectomy Educational Video Series
We have created a great 9 part video series that will provide you with a complete understanding of His Choice Vasectomy.
For more detailed information: His Choice Vasectomy educational video series
——
Total cost of single visit vasectomy procedure $1,250
The total charge for the single visit vasectomy procedure is $1,250 .
The $1,250 costs is all-inclusive and covers the entire vasectomy procedure and the three (3) month post-vasectomy semen analysis when performed in our office. If you prefer to take your semen sample to a local lab for evaluation then you will have to pay for the cost of an independent semen analysis.
Ready to get started?
Use this link to start scheduling: Scheduling a single visit vasectomy procedure
Cost of optional or mandatory vasectomy consultation visit $250
The cost for the vasectomy consultation visit is $250. You will have to call our office to schedule a consultation visit.
The consultation visit is optional and not required for most men. The consultation visit is only required for men who have a history of undescended testicle (either surgically corrected or uncorrected), who are on prescription blood thinners, or who have a bleeding disorder.
- If you would like a vasectomy consultation then the cost of the consultation will be $250.
- When you return for a vasectomy procedure you will be expected to pay $1,250 for the vasectomy procedure or $2,885 for the sedation vasectomy procedure.
Why is the consultation optional?
Over 95% of men will choose to have a single visit vasectomy procedure because 1) they are confident in their decision to not have any children or any more children and 2) our website has detailed information on the risks and benefits of vasectomy.
Some men don't feel comfortable with a single visit and would prefer to meet with Dr. Monteith before their vasectomy, discuss the procedure in person, and have specific questions answered. If you are one of these men, then we encourage you to schedule a consultation visit first.
The consultation visit is recommended when:
- Men have not fathered children
- Men are uncertain about their decision to have a vasectomy
Then two situations above increase the chance you may regret your vasectomy in the future. Talking about it with Dr. Monteith may help your decision making process.
The consultation visit is required when patients:
- Have a history of undescended testicle (either surgically repaired or not repaired)
- Are taking prescription blood thinners or history of bleeding disorders
Undescended testicle. This condition requires more complex medical decision making. Each patient's situation can be different. A scrotal exam can allow me to better predict the difficulty and risk of a vasectomy procedure. In some cases, the vasectomy may be more difficult on the surgically corrected side. In some cases, successful vasectomy may not be possible on the surgically corrected side.
Prescription blood thinners or history of bleeding disorders. These situations increase the risk of a bleeding complication (scrotal hematoma) during vasectomy. You may be able to avoid a consultation appointment if your doctor faxes their recommendations on how to manage your blood thinner before and after your vasectomy.
Patients who are on blood thinners can contact the doctor who prescribes the blood thinning medication and inform them they would like a vasectomy. For patients at low risk of forming a blood clot, your doctor may be able to complete a standardized form letter with recommendations about stopping your blood thinner and fax it to our office. Hematologists are very accustomed to these requests from their patients.
Ideally, patients should not be on a prescription blood thinner for 48 hours before their vasectomy. Some medications may require a longer time to clear your system before having a vasectomy.
Some medical conditions are minor and you can safely stop your blood thinner...some medical conditions are so serious that stopping your blood thinner, even for a short time, could cause you to form a life-threatening blood clot.
***Never stop your prescription blood thinner without consulting your prescribing doctor.***
If your doctor is uncomfortable providing you with a recommendation before vasectomy or you have a very high risk medical situation then a consultation appointment before the vasectomy is mandatory to decide if vasectomy is safe for you.
Ready to get started with a consultation?
If you want a consultation appointment then call our office to schedule.
Cost of sedation vasectomy procedure $3,150
If you request a sedation vasectomy procedure then the total charge for a vasectomy procedure under sedation is $3,150.
More information: Sedation Vasectomy Explained
You will need to pay the entire cost at the time you schedule your procedure.
The above costs covers the single visit Deep Sedation Vasectomy Procedure, surgery facility fee, nursing time, anesthesia staff time and anesthesia medications, and the three (3) month post-vasectomy semen analysis when performed in our office.
If you would like a consultation prior to your Deep Sedation Vasectomy Procedure, then there will be an extra cost for the consultation (see Cost of Consultation below).
Please be aware of the following items regarding Sedation Vasectomy:
- Single visit sedation appointments are available
- The consultation visit is optional
- If you have one of the conditions listed above the consultation appointment is required
- The sedation scheduling fee is not refundable
- The entire sedation vasectomy fee must be paid at the time of scheduling
- A driver is required on the day of your procedure
- We arrange our surgery schedule to accommodate your procedure. If you attempt to reschedule or cancel your procedure within seven (7) days of the scheduled date you will be charged a $500 rescheduling/cancellation fee.
Sedation vasectomy is not required for men to have a vasectomy, but neither is flying first class nor sitting in a luxury box at a sporting event!
Some men prefer sedation vasectomy for an additional guarantee of comfort during their vasectomy.
Ready to get started with Sedation Vasectomy?
If you are ready to schedule sedation vasectomy then use the link below
Start Scheduling Sedation Vasectomy
If you have any questions about scheduling then please call us at (919) 977-5060
Important Points About Sedation Vasectomy
- Single visit sedation appointments are available
Sedation vasectomy only offerred at our Raleigh, North Carolina office - Health Insurance is not accepted
- Full payment is required with 24 hours of scheduling
- A driver is required
- You must not eat or drink for 8 hours before the procedure
What health insurance plans we accept?
We DO NOT ACCEPT health insurance as payment for vasectomy. Not a single plan.
More information: Instructions on obtaining vasectomy reimbursement from your health insurance company
We will show you how to obtain reimbursement from your health insurance company after your vasectomy procedure has been completed.
It has simply become too burdensome (in time and emotion) to be in the middle of you and your health insurance company....it's a tough place to be....kind of like being a bull in a bull fight. How is it like a bull fight? Watch this video below to understand.
You will need to pay for your vasectomy on the day of your visit. We will provide you with a receipt and the billing paperwork and you can submit these directly to your health insurance company for reimbursement.
If you are uncomfortable with us not accepting your health insurance then you have (3) three options:
- Option #1.
Don't get a vasectomy. If you have an unplanned pregnancy then the next two options will not seem so bad. - Option #2.
Have your vasectomy with us. You will have a great vasectomy done in a single visit with a skilled provider offering the most minimally invasive vasectomy procedure. You can submit your receipt directly to your health insurance company after your procedure has been completed and be reimbursed directly by your health insurance company. - Option #3.
Go to another vasectomy provider. You will have two visits, may wait 1 to 4 weeks before each visit. You may have an office co-pay for each visit. You may have a group counseling session. You may be charged more for your vasectomy procedure. The average charge for a vasectomy procedure is $1,200 in North Carolina and $2,500 in Virginia. You may not have vasectomy coverage or you may have coverage but a high deductible. If you have a great health insurance plan, you will have two visits and at least 1 or 2 office co-pays. If you have a high deductible plan, have no vasectomy coverage, or don't have health insurance then you will have 2 visits and you will pay the full amount.
Why don't we accept health insurance for vasectomy?
Health insurance companies have consistently provided us with inaccurate information regarding an individual's coverage and how much a patient may owe. After the procedure has been completed, health insurance companies will occasionally inform us the information they provided during pre-verification was inaccurate; for example, they will say a person is fully covered or has to pay a specific amount. Several weeks after the procedure, the health insurance company will then tell us they made a mistake, the procedure was not covered and the patient needs to pay more.
Our office is then put in the awkward position of having to contact the patient and ask for more money. Often these calls are not well received. We are usually placed in the middle and the health insurance companies try to distance themselves from the problem they caused because their staff provided inaccurate information. Our office is then usually required to take the loss...even though we had nothing to do with the confusion.
We consistently have good reviews from patients. When we do have dissatisfied patients it is usually because their health insurance company provided inaccurate information. These patients often unfairly blame our office for the mistakes made by their health insurance companies.
Please keep in mind... health insurance is a business. You, the patient, are their client. You pay them money every month. They are more likely to be responsive to you, their client, rather than to me, the doctor.
Payment options for vasectomy: FSA/HSA, CareCredit, Advance Care
You will need to pay for your vasectomy on the day of your visit. We accept all major credit cards*, debit cards*, Flexible Spending Account (FSA)*/ Health Savings Account* (HSA) cards, AdvanceCare card* (see below) and cash.
*Please be aware there is a 3.99% credit card processing fee charged to any card payment swiped on our office terminal. This fee is charged by the credit card processor.
We do not accept cash, personal checks, cashier's checks, or money orders.
Vasectomy Financing
CareCredit
 CareCredit is a leader in the field of medical financing. CareCredit is a healthcare credit card designed for your health and wellness needs for you, your entire family and your pets.
CareCredit is a leader in the field of medical financing. CareCredit is a healthcare credit card designed for your health and wellness needs for you, your entire family and your pets.
More information: Apply for the CareCredit card
You can use your CareCredit card to pay for out-of-pocket expenses not covered by medical insuranceuch as tubal reversal, Essure reversal , and special financing options are available that you may not be able to get with other credit cards.
CareCredit offers a variety of financing options. You will need to apply for CareCredit directly from their website. You will need to go through a credit approval process to see if you qualify.
Advance Care
We accept the Advance Care card if you would like to finance your vasectomy.
The Advance Care card is a great way to get your vasectomy now and pay later. The application is simple and you can schedule your vasectomy as soon as you receive your card. The card looks and works just like a credit card.
 Approved applicants may receive up to 14 months of interest free financing at very competitive interest rates.
Approved applicants may receive up to 14 months of interest free financing at very competitive interest rates.
More information: Apply for the Advance Care Card
Please be aware the Advance Care card looks and acts just like a credit card but can only be used at approved medical providers.
—-
Step 1. Would you like a single visit vasectomy or vasectomy consultation appointment?
Would you like a SINGLE VISIT vasectomy appointment or a vasectomy CONSULTATION appointment?
Consultation are only required for men who have high risk medical conditions. You will need a consultation before having a vasectomy if you:
- Have a history of an undescended testicle
- Are taking a prescription blood thinner
- Have a bleeding disorder
If you have one of the above high risk conditions then you are required to have a consultation before you can schedule. Please call (919) 977-5060 to discuss.
Some men are not comfortable having a vasectomy in a single visit and would prefer a consultation visit first to discuss if vasectomy is right for them.
Over 95% of men choose to come for a single visit vasectomy procedure appointment. By carefully reading the website you should understand:
Our vasectomy videos are very informative. If you take the time to watch these videos you will obtain an extensive education about vasectomy. To view: Dr. Monteith's vasectomy educational video series
For more information: Good reasons to schedule a consultation appointment
If you would like to schedule a single visit vasectomy then proceed to Step 2 below.
If you are tying to schedule Sedation Vasectomy or a vasectomy consultation before having your vasectomy then call (919) 977-5060 to speak with a staff member.
Step 2. Select appointment date and time. Pay scheduling deposit.
To start scheduling your single visit vasectomy procedure complete the scheduling link below.
The scheduling link will allow you to select a date and time for your appointment. After you select a date and time, you will need to answer a scheduling questionnaire and then pay the scheduling deposit. Only after the scheduling deposit is paid will your appointment date and time be finalized.
Appointment Scheduling Deposit
A $150 appointment scheduling deposit is required because we offer single visit appointments. We want you to honor your commitment to keep your selected appointment time.
The scheduling deposit will be deducted from the total cost of your vasectomy procedure on the day of service.
- The scheduling deposit is fully refundable if you cancel your appointment seven (7) or more calendar days before the appointment
- The scheduling deposit is not refundable if you don’t cancel your appointment or if you reschedule or cancel within seven (7) calendar days of your appointment
To start scheduling a single visit vasectomy with Dr Monteith in his Raleigh office use the link below:
Dr Monteith: Single Visit Vasectomy His Choice Raleigh
Dr. Matthew Zerden is now offering His Choice Vasectomy in the Durham/Chapel Hill area. He does offer vasectomy appointments on select Saturdays and varying days of the week.
If you would like to schedule your vasectomy procedure with Dr. Zerden in his Durham/Chapel Hill office then visit his website to schedule with his office using the link below:
Dr Zerden: His Choice Single Visit Vasectomy His Choice Durham Chapel Hill
Review on how to schedule your vasectomy using the link above:
- After completing registration, you will be asked to select a date and time for your vasectomy. Our scheduling app only lets you schedule within next 30 to 90 days.
- You will need to pay the scheduling fee before your appointment is scheduled.
- You will receive immediate text and email notifications once your appointment is scheduled.
- If your date and time is not available then bookmark the scheduling page and return when your desired date is 30 to 90 days away.
You will need to call our office (919) 977-5060 if you are trying to schedule 1) vasectomy consultation appointment first or 2) Sedation Vasectomy.
Step 3. Read instructions. Watch our great videos!
We want you to be prepared before your vasectomy. The following links should help better prepare you:
We have a comprehensive 9 part educational vasectomy video series. If you watch this entire series of videos you will have the most extensive education we can provide:
—
AAAHC accredited facility
Our facility is accredited by Accreditation Association for Ambulatory Health Care. Your surgical procedure will be performed in a dedicated operating room located within our specialty center. For more information: Our facility
You will be cared for by nursing and anesthesia staff dedicated to your personal safety and the success of your procedure.
General anesthesia
We perform vasectomy reversal under general anesthesia in an operating room located within our office. The average vasectomy reversal surgery lasts 1.5 to 3 hours and is performed under general anesthesia provided by dedicated anesthesia staff.
Minimally invasive vasectomy reversal
Dr. Monteith performs minimally invasive vasectomy reversal. This vasectomy reversal procedure utilized by Dr. Monteith applies the same minimally invasive techniques used during No scalpel vasectomy; one small opening in the skin that does not require skin sutures to close.
During a minimally invasive vasectomy reversal a single opening less than 3 cm is created in the center of the scrotum using a no-scalpel dissector. The entire vasectomy reversal is performed through this opening and very often sutures are not required to close this opening.
As a result of a single, smaller opening not requiring sutures patients will often report minimal discomfort after reversal.
—-
Vasectomy reversal success: Time is the single most important factor
The time which has elapsed after the vasectomy if the most important factor on the success of the reversal procedure.
Sperm are continually produced in the epididymis after a vasectomy and travel up the vas deferens. After a vasectomy, the sperm will be trapped in the lower portion of the vas deferens with no egress. These sperm will slowly be recycled and reabsorbed by the man's body but this process will increase the pressure in the lower end of the vas deferens and the epididymis. This backpressure can cause gradual changes in the epididymis which can either cause additional blockages or can gradually cause the epididymis to become dysfunctional.
After vasectomy and with the passage of time these changes can become more pronounced and can decrease the success of vasectomy reversal.
Reversal less than 3 years of vasectomy, reversal success is 97%
Reversal within 3 to 8 years of vasectomy, reversal success rate is 91%
Reversal within 9 to 14 years of vasectomy, reversal success rate is 82%
Reversal 14 years or more after vasectomy, reversal success rate is 69%
The average success of restoring sperm to the ejaculate of all vasectomy reversal procedures is approximately 85%.
—–
Where are vasectomies reversed?
All vasectomy procedures are reversed in a state of the art operating room located within our facility.
Our operating room is dedicated to sterilization reversal for both men and women. This allows us to offer a personalized service, which is efficient, safe, and affordable. Our staff is dedicated to the care of patients who are reversing sterilization.
 Vasectomy reversal is performed under general anesthesia for patient's maximal comfort. Our anesthesia staff are dedicated to our practice and are able to devote their undivided attention to each of our patients. Anesthesia is administered using an Aestiva 5 anesthesia machine and isoflurane and sevoflurane are our anesthetic agents of choice.
Vasectomy reversal is performed under general anesthesia for patient's maximal comfort. Our anesthesia staff are dedicated to our practice and are able to devote their undivided attention to each of our patients. Anesthesia is administered using an Aestiva 5 anesthesia machine and isoflurane and sevoflurane are our anesthetic agents of choice.
The operating room is equipped with state of the art equipment including; Maquet halogen lighting, Maquet operating room table, centralized oxygen and vacuum, and multiple patient warming devices.
We have dedicated surgical technicians and surgical nurses who will make your experience safe and efficient. We have the latest Aesculap microsurgical instruments and sterilization instrument cases. All instruments are processed, cleaned, and sterilized in our facility by specially trained staff using modern instrument washing systems and vacuum steam sterilization autoclaves.
How is vasectomy reversed?
I use the same minimalistic surgical approach to vasectomy reversal as I do with my minimally invasive no-scalpel vasectomy procedures.
I make a single midline vertical skin incision in the scrotal skin. This incision is approximately one (1) to two (2) inches in length and very often will not require any suture to close.
For magnification I use high-resolution eye loupes which offer 6X magnification. The ends of each vas deferens are identified and opened. Using a German engineered nerve transector a perfectly flush right angle dissection is performed across each closed end of the vas deferens.
Each vas deferens is reapproximated under magnification using fine 9-0 microsurgical sutures in multiple layers.
The scrotal incision will often close on its own and will usually not require any sutures.
Patients recover in our recovery room for about an hour. They are then discharged to one of two specially selected hotels located within one-half mile of our office and in a central part of midtown Raleigh.
Patients then return to see me the next day for a post-operative evaluation. They are then free to return home, they may return to light duty within seventy-two (72) hours, and can resume sexual intercourse two (2) weeks after surgery.
—–
—-
Failure to achieve pregnancy
The main risk of vasectomy reversal is future pregnancy may never happen naturally.
The vasectomy reversal may be perfectly performed, without any complications, and sperm may reappear in the ejaculate in sufficient numbers to cause pregnancy but pregnancy may never occur.
Preexisting male infertility
Many men will have a vasectomy before having any children or a small number of children. Some of these men may have had undiagnosed male infertility or sub-optimal male fertility before their vasectomy. When these men have vasectomy reversal the factors contributing to male infertility will continue to be present.
Vasectomy induced epididymal dysfunction
The most common reason this can occur is because the epididymis in some men may become dysfunctional after a vasectomy. The epididymis is thought to become dysfunctional because of increased pressure caused by the continual production of sperm after the vasectomy that have no where to exit. This causes increased back pressure in some patients and over time this pressure can cause gradual dysfunction of the epididymis. The epididymis may cease producing sperm or produce dysfunctional sperm.
Formation of anti-sperm antibodies
Some men will form immune reactions against their own sperm after vasectomy and will form antisperm antibodies. The contribution of antisperm antibodies to male infertility and sperm dysfunction is controversial because many men may develop antisperm antibodies; however, most will not have infertility or sperm dysfunction.
Combinations of these issues can also contribute in an additive fashion to the insufficient reappearance of sperm in the ejaculate.
Female infertility
Equally possible is the vasectomy reversal may be 100% successful but the female partner may be the source of infertility. The most common conditions found in women as a cause for infertility are not ovulating (releasing eggs) regularly, blockage of the fallopian tubes, and difficulty conceiving because of increasing maternal age.
Some couples will have everything working perfectly and not be able to become pregnant because of unexplained infertility.
Occlusion of the vas deferens
The vas deferens may heal with scar tissue and be blocked at the repair sites.
The inside of the vas deferens is delicate and small. If the repair site heals aggressively with scar tissue then the inside of the vas deferens may be blocked and sperm may not be able to be transported to the seminal vesicles.
One or both of the vas deferens could heal closed with scar tissue. If blockage occurs in only one vas deferens and the other heals without blockage then sperm will often reappear in the ejaculate in adequate enough amounts to cause pregnancy. Very often men who have one open and fully functioning vas deferens will have normal sperm counts.
The chance of one or both of the vas deferens healing with blockage is 3-10%.
Hematoma formation
A hematoma is a collection of blood that forms a localized blood clot and can occur after any surgical intervention.
Arterial hematomas occur rapidly and often in less than twelve (12) hours after a vasectomy reversal. Venous hematomas occur less quickly and usually within 24 to 36 hours. Small hematomas may cause pain and discomfort but can be reabsorbed by the body without surgical intervention. Large hematomas will cause pain and discomfort and will require surgical evacuation.
The risk of hematoma formation after vasectomy reversal is less than 5%.
Infection
Infection is possible after any surgical procedure. If an infection were to occur after vasectomy reversal it can often be treated with oral antibiotics but may require hospitalization. If an infection persisted an abscess could (form) and hospitalization and drainage may be required.
The overall risk of infection after vasectomy reversal is less that 3%.
Bleeding
Bleeding is a possible complication of almost any surgical intervention.
Vasectomy reversal requires more surgical manipulation of the vas deferens and the risk of bleeding after vasectomy reversal is likely higher than with vasectomy. Bleeding risk are increased if the patient is on a blood thinner, has a bleeding disorder, or has scar tissue from previous scrotal surgery or infection.
Overall the risk of serious bleeding during or after a vasectomy reversal is less than 1%.
Chronic pain
Most cases of chronic pain after vasectomy reversal are mild and cause minimal disruption to a patient's daily life. Granulomas (small collections of sperm) or neuromas (abnormally healing nerves) are thought to be the cause of most of these cases of mild but chronic pain after vasectomy reversal.
Chronic, severe testicular pain is a rare but possible risk of vasectomy reversal.
This complication can occur after any surgical manipulation of the testicles or vas deferens (vasectomy or vasectomy reversal) but can also occur after surgery to other areas of the male genitourinary tract. The cause for severe, chronic pain is unclear but is felt to be caused by changes in the nerves during the healing process after surgery. This complication is poorly understood.
The estimate of chronic pain after vasectomy reversal is difficult to determine but should be less than 1%.
Testicular atrophy
Testicular atrophy is a rare but possible risk of vasectomy reversal.
This complication is caused by repeated insult to the blood supply of the testicle. This can occur in patients who have had multiple scrotal surgeries and the risk may be increased in patients who have underlying disorders of the circulatory system.
The risk of testicular atrophy after vasectomy reversal is less than 0.5%.
—
Patient age : Most important predictor of tubal reversal success
The age of the woman at the time of tubal ligation reversal is the single most important predictor of tubal reversal success. Why?
Although pregnancy is always possible if a woman is having regular periods, the ability for a women to become pregnant declines with increasing age. The power of tubal ligation reversal is that it allows women the chance to become pregnant every month. The more chances one has (i.e. the more months) then the higher the chance of pregnancy. A woman who has tubal reversal at the age of 36 has a much higher chance of pregnancy than does a woman who has tubal reversal at the age of 45. The more months you allow it to work then the higher the chance of pregnancy.
The chance of pregnancy after tubal ligation reversal when the woman is less than 30 years of age can be as high as 80% and the chance of pregnancy after reversal when the woman is over 40 years of age is approximately 35%.
Most of our patients will become pregnant within 12 months of having tubal reversal surgery.
Type of tubal ligation: Second most important predictor of tubal reversal success
The type of tubal ligation being reversed is the second most important predictor of the chance of pregnancy success after tubal reversal surgery.
All tubal ligation procedures cause blockage in the tube. Some tubal ligations cause blockage with minimal damage to the fallopian tube (tubal clips and tubal rings). Other types of tubal ligation cause varying amounts of damage to the fallopian tube and are more dependent on the surgical techniques of individual physicians: ligation and resection (tying and cutting) and coagulation (burning). Newer forms of tubal ligation (Essure) cause tubal blockage inside the fallopian tube.
Tubal ligation reversal pregnancy success can be as high as 80% with reversal of tubal clips and rings and as low as 35% with reversal of Essure. Tubal reversal pregnancy success is approximately 65% with reversal of tubal coagulation.
—
Tubal clips: Filshie and Hulka clips
A common method of tubal ligation is Filshie or Hulka clip tubal occlusion. Tubal clip ligations are often performed six (6) weeks or more after pregnancy and delivery. These procedures or often performed laparoscopically (small camera inserted through the belly button). Occasionally tubal clips can also be applied directly to the tubes during a c-section.
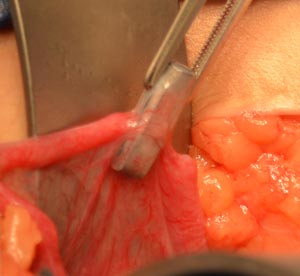
Tubal clips cause blockage of the tube by exerting pressure on a small section of the tube. This causes the blood supply to that area to decrease and the tissue undergoes changes which result in the tube healing closed and separating. The tubal clips serve no function after the tubal ends have closed and separated.
Tubal clips are an excellent tubal ligation method for reversal and reversal of clips often provides the highest chance of pregnancy success. Why?
Compared to other tubal ligation methods, fallopian tube clips only damage a very small portion of the fallopian tube when they cause tubal blockage. It is technically easier to rejoin the tubal segments because the sections of fallopian tube are more similar in size.
When we repair a clip tubal ligation we are often more certain the remaining fallopian tubes will be healthy and long. In comparison to other tubal ligation methods, the performance of clip tubal ligation is more similar among doctors than ligation and resection (cutting and tying) or coagulation (burning). This means the technique is fairly consistent among doctors and the reversal results are more predictable.
Many mistakenly believe reversing clips is as simple as just removing the clip and the tube will be reopen. Unfortunately it is not quite that easy. The clips have to be removed, the closed ends opened, and the tubal ends rejoined using microsurgical techniques.
Pregnancy success after reversal of tubal clips can be as high as 80%.
Tubal rings: Falope, Yoon, Silastic bands
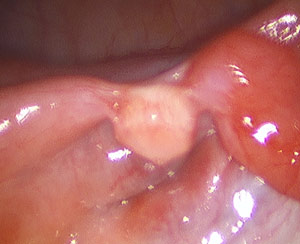
Tubal ring tubal ligation is also a common method of tubal ligation which causes minimal damage to the fallopian tubes. Tubal clips are often applied during a laparoscopic (small camera inserted in the belly button) procedure.
Similar to tubal clips, tubal rings are an excellent method for tubal reversal.
Tubal rings cause blockage of the fallopian tube in a manner similar to tubal clips. Tubal rings do damage slightly more of the fallopian tube than tubal clips but this does not seem to adversely impact pregnancy success rates after reversal.
As with tubal clips, reversal of tubal rings cannot simply be performed by removing the rings. The rings cause the tubal ends to heal closed and the ends will separate. To reverse the effects of tubal rings, the rings must be removed, the tubal ends reopened, and the fallopian tube ends rejoined with microsurgical techniques.
Pregnancy success after reversal of tubal rings can be as high as 80%.
Cutting and tying: Pomeroy, Parkland, Irving, and Uchida
When tubes are cut and tied during a tubal ligation the more correct term for this method is ligation (tying) and resection (to remove by cutting). This is a very common method of tubal ligation when performed during a c-section or within the first 24 hours after a vaginal delivery.
Although most people are aware of the concept of cutting and tying tubes very few people actually understand the exact reasons for each step. A small segment of the tube is tied first before it is cut. The purpose of the suture is to prevent bleeding. The tube will then be cut to cause physical disruption of the fallopian tube. The suture will eventually be absorbed and the closed ends of the tubes will separate.
Ligation and resection methods are reversible and with good success but this method is more dependent on the different techniques of individual doctors. Some doctors remove minimal amounts of tube and others may remove larger amounts, the ends of the tubes, and, in rare cases, both tubes in their entirety.
It is helpful for us to review the operative and pathology reports of these types of tubal ligation so we can determine both the technique and the amount of tube removed by a patient's doctor.
Pregnancy success after reversal of ligation and resection averages 66%.
Burning: Bipolar and monopolar coagulation
Tubal coagulation is also known as tubal burning. Although this method sounds like an extreme way to cause tubal blockage it is very common, despite popular opinion, is also very reversible if the doctor did not burn too much of the tube.
Tubal coagulation exists in two forms: bipolar and monopolar coagulation. Bipolar is the most common type and is the least destructive of the two.
Tubal coagulation is often performed during a laparoscopic procedure (camera inserted through the belly button). It is very typical for a doctor to perform a one (1) to two (2) cm burn or to burn the tube in 3 (three) adjacent spots.
Burned tubes can often be successfully repaired but this method is dependent on the technique of individual doctors. Some doctors will coagulate small amounts and other will coagulate larger amounts. Some will coagulate the tube close together
Pregnancy success after reversal of tubal coagulation averages 66%.
Hysteroscopic tubal occlusion: Essure sterilization
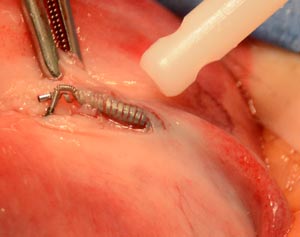
Essure is a newer sterilization procedure which causes occlusion (blockage) of each fallopian tube from the inside.
During the Essure procedure a micro-insert device composed of two coils is inserted into the very opening of each fallopian tube from inside the cavity of the uterus. The micro-insert device causes scar tissue to form inside the fallopian tube and this causes permanent blockage of each tube.
We were the first physicians in the world to publish case reports on successful pregnancy after outpatient Essure reversal. Essure can be reversed by surgically removing the coils and then re-inserting the remaining healthy fallopian tube into the cavity of the uterus.
The chance of pregnancy after reversal of Essure sterilization is approximately 35%.
—-
Tubal ligation reversal
In our experience we can reverse tubal ligations in over 98% of patients who will come to our center.
The chance of pregnancy after tubal reversal depends on the age of the patient, the type of tubal ligation, and the health of the remaining fallopian tube.
In general about 2 out of every 3 patients become pregnant after tubal ligation reversal surgery. The average pregnancy success rate is 60% to 70%.
- Cash discounted cost for tubal reversal surgery is $7,500
- Cost of a financed reversal surgery is $8,100
Most health insurance plans will not pay for tubal reversal surgery....no matter what the reason. The majority of health insurance plans consider both in vitro fertilization and tubal ligation reversal elective treatments...which means treatments that are not medically required.
When having tubal ligation reversal you will need to plan on paying out of pocket for your surgery. His Choice works with two major health care financing companies that can help you cover the cost of tubal ligation reversal surgery.
Most patients will pay in full when having surgery. Others will either finance surgery or start a reversal prepayment savings plan.
Essure removal
For women who have Essure sterilization and then develop abnormal symptoms we offer removal of the Essure micro-insert devices.
The majority of our patients who have Essure removal will experience improvement in their symptoms.
- Cash discounted cost for Essure removal surgery is $8,500
- Cost of a financed Essure removal surgery is $9,100
It is more common for health insurance to pay for Essure removal. As of December 2019, Essure was withdrawn from the US health care market because of increasing litigation because of Essure side effects and Essure associated complications.
Your health insurance may pay for Essure removal but only only with the following circumstances:
- Essure removal will need to be performed in a hospital setting.
- Your doctor will either have to remove your fallopian tubes completely (complete salpingectomy) or remove your uterus (hysterectomy). Your doctor will not be able to perform an Essure reversal (restoration of normal anatomy allowing you the chance to become pregnant). Most doctors have limited experience with Essure removal and very little knowledge of Essure reversal.
Our office performs Essure removal safely in an out-patient operating room. We perform 2 to 4 of these procedures every week and have done so since 2008. We have extensive experience is safely removing the devices with a low risk of fracture.
We are unable to accept health insurance for Essure removal or Essure reversal. You may be able to get partial reimbursement for your Essure removal procedure after your surgery has been completed but you will need to pay in full before your surgery and apply for reimbursement from your health insurance company after your surgery has been completed.
Essure reversal
For women who have Essure sterilization and who wish to become naturally pregnant we offer Essure reversal surgery. We were the first physicians to report successful pregnancy after outpatient reversal of Essure sterilization.
- Cash discounted cost for Essure reversal surgery is $8,500
- Cost of a financed Essure reversal surgery is $9,100
We have extensive experience with Essure reversal surgery. We can perform the surgery under general anesthesia in an out-patient surgical setting. The surgery averages 80 minutes in duration. The chance of pregnancy success averages 30% to 40%.
Screening laparoscopy
Our center is unique in many ways. On major difference is we offer our patients an optional screening laparoscopy procedure.
If patients do not have their tubal ligation records or desire more certainty about the reversibility of their tubal ligation then they can choose to have a screening laparoscopy procedure. During a screening laparoscopy, a small camera is inserted into the umbilicus (belly button) and the fallopian tubes are closely examined.
- Cash discounted cost of the screening laparoscopy $2,500
- Cost of financed screening laparoscopy is $3,100
The laparoscopy is optional. It can be best thought of as a surgery insurance policy. If patients choose a screening laparoscopy and their tubes are not repairable then they are offered a significant refund of their surgical fee.